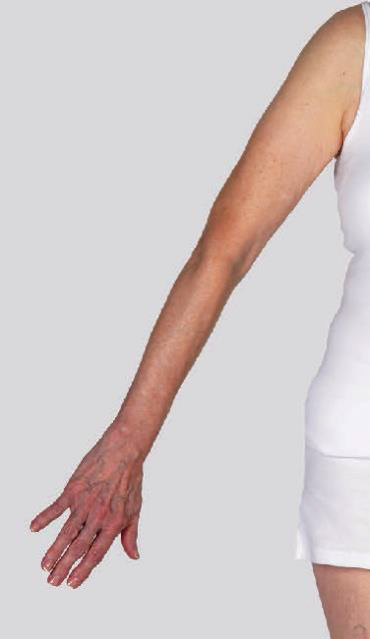
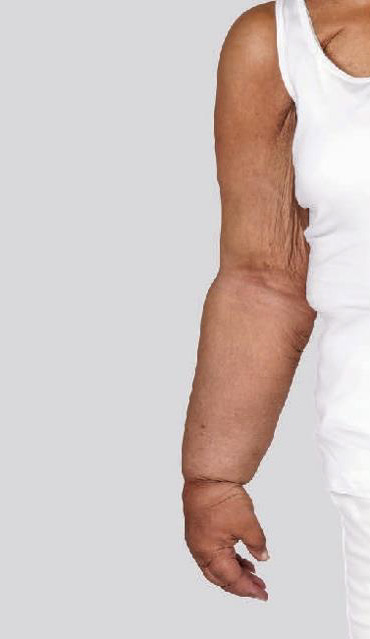
Types of lymphedema
Lymphedema can be either primary or secondary. Primary lymphedema occurs on its own, usually as a result of a genetic condition. Secondary lymphedema—the most common type—occurs as a response to another condition, such as an infection, injury, trauma, cancer or cancer treatment.